Audiology research answers important questions about the causes, experiences, best management and service provision for people with hearing loss, tinnitus and balance problems. It provides the scientific foundation upon which clinical decisions and practices are built within the field of Audiology.
Why is research important in Audiology?
There have been many important discoveries in Audiology that have directly informed our current clinical practice.
However there are many unanswered questions in Audiology, and much of our clinical practice has a limited evidence base. There is less Audiology related research compared to other specialities, and “Ear” research is the health category with the lowest expenditure, based on 2018 UK health research funding data.
The UK Action Plan for Hearing Loss and Tinnitus Research is currently being developed to identify a set of recommendations to grow Audiology related research in the UK, recognising the importance for patients and wider stakeholders of increasing research and innovation.
As well as generating new knowledge, there are other advantages to research.
- Involvement in research benefits patients. Evidence suggests that a strong research culture in an organisation appears to be associated with benefits to patients, staff and the organisation (Harding et al, 2017; Boaz et al, 2015).
- Involvement in research benefit departments. Research-active clinical departments have better staff retention and staff are more likely to recommend hospital organisations that are involved in research (Harding et al, 2017).
- Involvement in research benefits clinicians. Research involvement can improve clinician knowledge base, offer additional career opportunities, counting towards continued professional development, enhance consultations with patients through being better informed, strengthening skillsets of critical analysis, writing, planning and communication skills.
Different ways of being involved in Audiology research
There are many ways to get involved with research. You don’t have to lead and design a research project yourself. Research involvement can be a simple as keeping up to date with evidence– research awareness, to advertising opportunities to patients to take part in a project, involving minimal amounts of time – research facilitation, to something more complex such as being a principal investigator at your local site for a multi-centre study or running your own project – research leadership, or anywhere in-between.
Research Awareness

- Keeping up to date with new evidence
- Knowing what current research is being undertaken
- Applying new knowledge into practise
- Participating in conversations about research
Research Facilitation

- Offering opportunities to patients to get involved in research
- Advertising research studies in your department
- Consenting patients to take part in research
- Contributing expertise to the development of research protocols
- Measuring an outcome measure for a research study
Research leadership

- Being a principal investigator at your local site for a multi-centre study-leading research delivery
- Designing and running your own study
- Becoming a clinical academic
- Building a research culture and enabling audit, evaluation & research in your department
- Collaborating with researchers to design and conduct studies that address clinical relevant questions
What is it like to be involved in research – hear about the perspectives of allied health professionals, nurses and midwives across the different levels of involvement: https://healthtalk.org/experiences-nurses-midwives-allied-health-professionals-research/overview
The research process
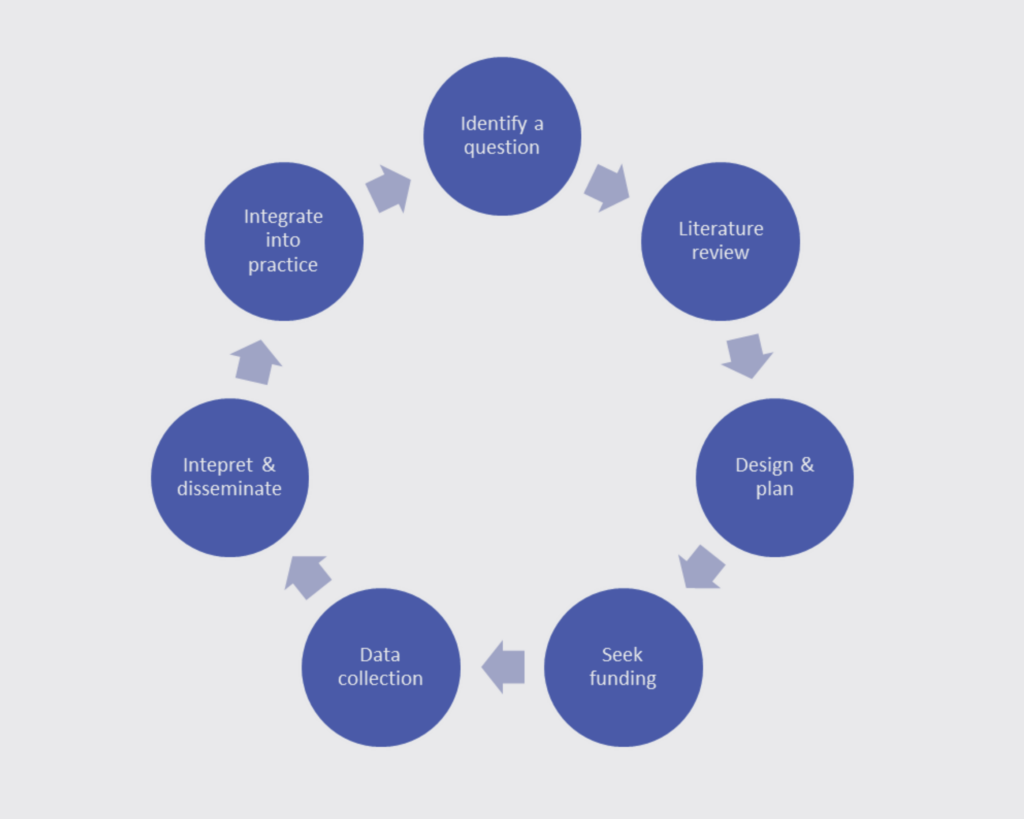
The research process typically begins with identification of a research question or topic, often guided by existing gaps in knowledge or areas of interest. A comprehensive literature review is required to examine prior studies and establish the context for their work. This informs the design of the research plan, the objectives, methodologies, data collection techniques, and analysis tools that will be used. This plan forms the basis of a funding application.
Once the research plan is finalised and all relevant approvals have been obtained, data is collected, often involving experiments, interviews, surveys, observations, or analysis of existing data sets. This data undergoes rigorous analysis, allowing researchers to draw meaningful conclusions and insights. The findings are then interpreted within the context of the research question, and the results are disseminated through publications, presentations, or discussions, contributing to the ever-evolving body of knowledge in the field.
Research is a team process
Audiology and healthcare research is not an individual pursuit and requires a team approach throughout the whole research process.
Who is potentially involved in the Audiology research team?
The Chief Investigator has overall responsibility for the research, and leads the team:
The team is likely to involve a number of different roles and professions:
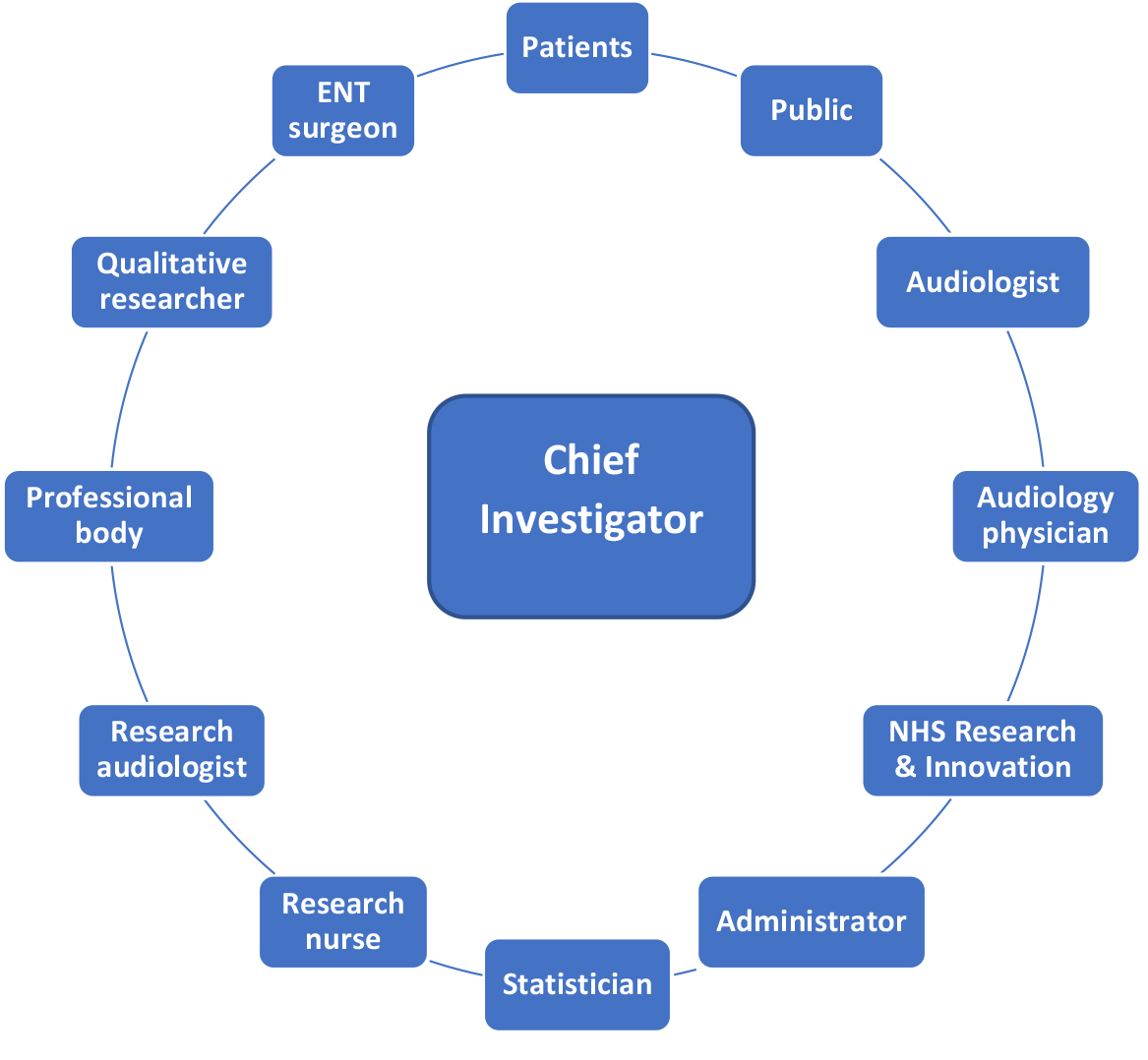
These are some of the different groups who may be involved in a research team. While not all groups may be represented in each research team, patients and/or the public should always be involved .
Why is this important?
A team approach ensures that:
- research questions being investigated are relevant and meaningful to patients, clinicians, commissioners and the public
- potential research findings will be of patient benefit and are likely to be implemented into practice
- the research is ethically sound
- the research is practical and feasible to be delivered within healthcare settings
- the research has been well designed to answer the research question
- there are appropriate resources available to carry out the research
- the data analysis will be high quality there is a collective of knowledge and skills to interpret the data
- the research findings are disseminated widely and reach the right audience
- the research findings can be implemented into practice
Team science
Enhances the likelihood that research findings will be clinically relevant and applicable, ultimately benefiting patients and improving healthcare delivery.
Find out more about involving patients and the public in research
Different types of research study designs
There are a wide range of study designs used in research projects, because different research questions require different approaches to gather the most relevant and reliable data.
Randomised controlled trial (RCT)

A randomised controlled trial is a scientific study design used to assess the effectiveness of new treatments, interventions, or methods in a controlled and systematic manner. This type of trial helps researchers determine whether a new approach to assessment, treatment, or intervention is truly beneficial compared to the existing standard practices.
Participants are randomly assigned to different groups to compare the effects of, for example, a new treatment method against an existing one. Random assignment helps balance out any differences between the groups, making the comparison more reliable.
The ACHIEVE study
An example of a recent RCT in Audiology is the Achieve (Aging and Cognitive Health Evaluation in Elders) study, from the US (Lin et al, 2023). This study “aimed to investigate whether a hearing intervention could reduce cognitive decline in cognitively healthy older adults with hearing loss”.
Older adults with hearing loss were randomly assigned to either have an audiological intervention and hearing aids, or a health education intervention which did not focus on hearing. The change in cognitive score between these two groups was examined after 3 years.
Spoiler alert: there was no difference in cognitive decline between the two groups.
Cluster randomised controlled trial

A cluster randomized controlled trial is similar to a RCT, but it tests the effectiveness of interventions or treatments in a way that makes sense for groups, or “clusters,” of participants rather than individual participants. Examples of clusters include clinics, schools or communities.
The FAMOUS study
An example of an ongoing cluster RCT in Audiology is the FAMOUS (study from the UK), funded by the NIHR
This study is aiming to investigate “What is the clinical and cost-effectiveness of follow-up and monitoring in new adult users of NHS hearing aids compared to usual care”
Cohort study

A cohort study is a type of observational research design to investigate the relationships between specific exposures or risk factors and the occurrence of certain outcomes or events over time. In a cohort study, a group of individuals, known as a cohort, is followed over a defined period to assess how different factors may influence their health outcomes. Cohort studies are particularly valuable for studying the causes of diseases, identifying risk factors, and tracking the development of diseases or conditions.
The Seashel Study
An example of a cohort study related to Audiology is the Seashel study. This study aimed to identify the characteristics of adult patients presenting to NHS ENT and hearing services with idiopathic sudden sensorineural hearing loss.
Qualitative research approaches

Qualitative health research is used to explore and understand various aspects of health, illness, healthcare systems, and the experiences of individuals within these contexts. Qualitative health research seeks to gather and analyse non-numerical data, such as narratives, interviews, observations, and textual documents, to uncover the meanings, perceptions, and social constructs related to health and healthcare.
There are different approaches to qualitative research, including:
Phenomenology
Phenomenological research aims to understand the lived experiences of individuals within a specific phenomenon or context. Researchers seek to explore the essence and meaning of those experiences. This approach is often used to study patient experiences, illness narratives, and the subjective aspects of health and illness.
An example of a phenomenological study is by Marks et al (2019). This study “explores the lived experience of chronic disabling tinnitus, with the aim of understanding how distress and chronicity occur, and what might help to reduce this”.
Grounded Theory
Grounded theory research focuses on developing theory from qualitative data. Researchers collect and analyse data to identify patterns, concepts, and categories that emerge from the data itself, rather than starting with preconceived theories. This approach is often employed to generate theories that explain social and healthcare processes.
An example of a grounded theory study is by Hughes et al (2018) who explored “the perceptions, understanding, and experiences of listening effort in adults with severe-profound sensorineural hearing loss before and after cochlear implantation”.
Ethnography
Ethnographic research involves immersing researchers in the field to gain an in-depth understanding of a particular culture, community, or healthcare setting. Researchers observe and interact with participants over an extended period, often using participant observation, interviews, and field notes to capture the cultural and social context of health-related phenomena.
An example of a study using ethnographic observations is by Pryce and Gooberman-Hill (2012), who aimed to explore “factors affecting communication with a hearing loss in residential care”.
Systematic review

A systematic review is a rigorous and comprehensive research methodology used to synthesise, analyse, and summarise existing evidence on a specific research question or topic. Systematic reviews are a critical component of evidence-based practice and policy-making in various fields, including medicine, public health, psychology, education, and social sciences. The primary aim of a systematic review is to provide an unbiased and reliable assessment of the available research studies to inform decision-making, clinical guidelines, or further research.
An example of a systematic review is by Maidment et al (2018) who aimed to explore “the perceptions, understanding, and experiences of listening effort in adults with severe-profound sensorineural hearing loss before and after cochlear implantation”.
What is the difference between research, service evaluation and audit?
- Research aims to generate new knowledge
- Service evaluation aims to assess the processes and outcomes of a clinical service
- Audit aims to determine whether a clinical service meets a defined standard
The Health Research Authority have a tool for understanding the difference.
While audit, service evaluation, and research are distinct activities with their own objectives and purposes, all three can overlap and the boundaries between them aren’t necessarily clear.
Audits and service evaluations often involve data collection and analysis, which may resemble research methods. They all require use of structured approaches to gather and analyse data. Ethical principles apply for audit and service evaluation, even if NHS ethical approval is not required. The extent of overlap depends on the specific goals and context of each activity.
Getting involved in audit and service evaluation is a good way to develop research skills and to build a research culture. The National Institute for Health and Care Excellence (NICE) have produced guidance and resources to support with clinical audit and service development.
Audit and service improvement | Into practice | What we do | About | NICE
Research organisations
There are many local and national organisations and networks that drive research within healthcare and it can be difficult to know who to go to or the roles of different organisations.
This video gives an oversight of how clinical research is structured in the UK:
Below is a list of some of the key organisations with a brief description.
| Organisation | Acronym | Description |
| National Institute for Health Research | NIHR | The largest funder of public health research in the UK to improve the health and wealth of the nation through research. |
| National Institute for Health and Care Excellence | NICE | Organisation aiming to improve outcomes for people using the NHS and other public health and social care services through the production of evidence-based guidance, quality standards, and information services. |
| Biomedical Research Centre | BRC | BRCs are collaborations between NHR Organisations and Universities, funded by the NIHR. They bring together academics and clinicians to translate scientific discoveries into potential new treatments, diagnostics and technologies. There are three BRCs with a hearing theme. |
| UK Research and Innovation | UKRI | UKRI is government funded and includes the 7 research councils, including:
Medical Research Council (MRC) Engineering and Physical Sciences Research Council (EPSRC) Economic and Social Research Council (ESRC) Biotechnology and Biological Sciences Research Council (BBSRC) |
| James Lind Alliance | JLA | The top 10 priorities for research in different fields are considered by patients and clinicians collectively and can provide good places to start when considering research questions that are timely, appropriate and most likely to make a difference to patients. |
| Clinical Research Network | CRN | There are 15 CRNs across England, which coordinates and supports the delivery of high-quality research. The CRNs provide a vast range of national and local resources and activities designed to support health and care organisations engage in research activities. |
| Health Education England | HEE | HEE works with partners to plan, recruit, educate and train the health workforce. In 2023, HEE was merged with NHS England. |
| Health Research Authority | HRA | Core purpose is to protect and promote the interests of patients and the public in health and social care research, overseeing a range of committees and services and ethical approvals of research. |
| Health and Care Research Wales | HCRW | Health and Care Research Wales is a networked organisation, supported by Welsh Government, HCRW works in close partnership with other government agencies and research funders (both in Wales and across the UK); industry partners; patients; service users; public and other stakeholders.
HCRW work together to promote research into diseases, treatments, services and outcomes that can lead to discoveries and innovations which can improve and even save people’s lives. |
| NHS Research Scotland | NRS | Promotes and funds clinical and translational research in Scotland in partnership with Scottish NHS Boards and Chief Scientist Office of Scottish Government. |
| Northern Ireland Clinical Research Network | NICRN | Funded by the Health and Social Care (HSC) Research and Development Division supports high quality clinical trials across all HSC Trusts and promotes research within NI, develops partnerships and relationships between individuals across the networks. |
| NIHR Research Support Service | RSS | The RSS provides researchers, especially those applying for and in receipt of NIHR funding, with free access to support, advice and expertise. It helps them develop and deliver clinical and applied health and care research. |
| Integrated Research Application System | IRAS | UK-wide system that streamlines the process for applying for permissions and approvals to conduct health and social care research. |
